The terms folate and folic acid are often used interchangeably, but don’t be fooled – they’re not the same!
Folate is the natural form of vitamin B9 found in foods, while folic acid is the synthetic form added to supplements and fortified or enriched foods.
The chemical structures of folate and folic acid are similar, but not identical, so there are differences in how they’re processed and used by our bodies.
In this article, we’ll discuss the structural and functional differences between folate and folic acid and which one is a better supplement choice for most people.
Want to save this article? Click here to get a PDF copy delivered to your inbox.
Clickable Table of Contents
Folate: The Natural Form of Vitamin B9
Sometimes, researchers use the term “folate” to refer to all forms of vitamin B9 (including folic acid).
However, for the purposes of this article, we will use “folate” to describe the form that is found naturally in food.
Natural Folate Metabolism
Natural folate exists in many different forms, but polyglutamates (folate molecules with a tail of several glutamates) are the most common (1).
In order to be absorbed, the glutamate tail must first be removed by enzymes located on the lining of the small intestine (also known as the brush border) (2).
After being absorbed into the cells of the small intestine, these folate molecules are converted to the active form of folate known as L-5-methyltetrahydrofolate (L-5-MTHF) or L-methylfolate:
After this process is complete, activated folate (L-5-MTHF) is released into the bloodstream where it can be distributed throughout the body, taken up by cells, and either metabolized or converted back to the polyglutamate form for storage.
The intestines are very efficient at converting natural food forms of folate into the active form, even at high doses, so there is no tolerable upper limit for natural food folate.
Folate’s Role in Health
The primary role of folate is to participate in one-carbon metabolism (3).
One-carbon metabolism is the transfer of one-carbon units, such as methyl groups (CH3), between molecules (4).
This process is necessary because one-carbon groups are too unstable by themselves and must constantly be attached to something.
One-carbon transfers are required for many metabolic processes, including amino acid metabolism, DNA synthesis, and cell division.
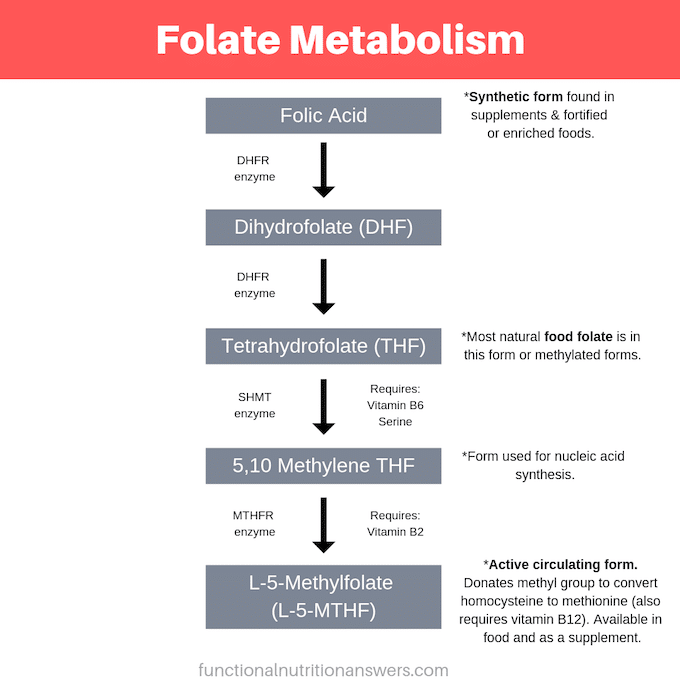
Here’s an overview of how the process works:
There are a few important steps to note:
1. Conversion of homocysteine to methionine.
First, you can see that folate (L-5-MTHF) donates a methyl group to homocysteine (a byproduct of protein metabolism) in order to form methionine (an amino acid that is required for growth and tissue repair) (4, 5).
If folate is not available to provide a methyl group for this conversion (or if there is not enough vitamin B12 as a cofactor), homocysteine can build up in the blood (6).
Elevated levels of homocysteine have been associated with increased risk of several chronic conditions, including heart disease and Alzheimer’s disease (7, 8).
However, interventions focused on lowering homocysteine levels have not consistently reduced the risk of these conditions, so it may be more of a risk marker than a direct cause of disease. More research is needed (9).
2. Formation of SAM and methylation reactions.
Second, methionine goes on to participate in methylation reactions, which are especially important for DNA synthesis and the regulation of gene expression (10).
Once methionine has been formed, it can be converted to S-adenosylmethionine (SAM), which is one of the body’s most important methylators.
SAM transfers a methyl group (CH3) to other molecules, like DNA or proteins, and participates in over 100 methylation reactions (3, 11).
Without enough folate to spur the one-carbon metabolism cycle, methylation reactions may be impaired throughout the body.
3. Recycling L-5-MTHF back to THF & nucleotide synthesis.
Finally, after L-MTHF donates a methyl group to homocysteine, it is converted back to THF.
From there, it can be converted again to 5,10-MTHF, the form of folate used to make nucleotides (the building blocks of DNA and RNA).
Thus, it is clear that folate is involved in many many important processes in the body.
Folate Deficiency
In the United States, folate deficiency is rare (<2%), but still possible (12).
Deficiency is most often caused by low-intake of folate-containing foods, but can sometimes be caused by malabsorption issues or medications as well (2, 13).
The most common sign that you might have a folate deficiency is megaloblastic anemia (although, megaloblastic anemia can also be caused by vitamin B12 deficiency, so it is important to rule that out too) (14).
Megaloblastic anemia is a condition in which red blood cells (RBCs) are too large (macrocytic), immature (megaloblastic), and low in number.
This occurs because a lack of folate impairs DNA synthesis and disrupts cell division within the bone marrow (where blood cells are formed). This leads to RBCs that aren’t formed properly or rapidly enough.
These megaloblastic RBCs result in blood that has a decreased oxygen-carrying capacity, which translates to symptoms like fatigue and shortness of breath (15).
Anemia isn’t the only consequence of folate deficiency – many other conditions have been linked with inadequate folate consumption, including the following:
- Alzheimer’s disease (16, 17)
- Autism spectrum disorders (18, 19, 20)
- Cancer (21, 22, 23)
- Cardiovascular disease (24, 25)
- Depression (26, 27)
- Dementia (28, 29, 30)
- Neural tube defects (31, 32)
Thankfully, folate deficiency can generally be avoided by consuming a diet rich in folate or by taking supplements as needed.
Foods High in Folate
Folate is found in many whole foods, especially poultry liver, legumes, and green vegetables.
Here are some of the foods with the highest amounts of folate (33):
- Turkey liver: 587 mcg (146% DV) per cooked 3 ounces
- Chicken liver: 491 mcg (122% DV) per cooked 3 ounces
- Edamame: 482 mcg (121% DV) per cooked cup
- Chickpea flour: 392 mcg (98% DV) per cup
- Cranberry beans: 366 mcg (92% DV) per cooked cup
- Roasted soybeans: 363 mcg (90% DV) per cup
- Lentils: 358 mcg (90% DV) per cooked cup
- Black-eyed peas: 358 mcg (90% DV) per cooked cup
- Wheat germ: 323 mcg (80% DV) per cup
- Mung beans: 321 mcg (80% DV) per cooked cup
- Sunflower seeds: 319 (79% DV) per cup
- Adzuki beans: 317 mcg (79% DV) per cooked cup
- Pinto beans: 294 mcg (74% DV) per cooked cup
- Pink beans: 284 mcg (71% DV) per cooked cup
- Chickpeas: 282 mcg (71% DV) per cooked cup
- Baby lima beans: 273 mcg (68%) per cooked cup
- Spinach: 263 mcg (66% DV) per cooked cup
- Black beans: 256 mcg (64% DV) per cooked cup
- Navy beans: 255 mcg (64% DV) per cooked cup
- Yardlong beans: 250 mcg (62% DV) per cooked cup
- White beans: 245 mcg (61% DV) per cooked cup
- Asparagus: 243 mcg (60% DV) per cooked cup
- Mustard spinach: 238 mcg (59% DV) per raw cup
- Kidney beans: 230 mcg (58% DV) per cooked cup
- Conch: 227 mc (56% DV) per cooked cup
- Beef liver: 221 mcg (55% DV) per cooked 3 ounces
- Avocado: 205 mcg (51% DV) per cup
- Artichokes: 200 mcg (50% DV) per cooked cup
- Pigeon peas: 186 mcg (46% DV) per cooked cup
- Peanuts: 185 mcg (46% DV) per roasted cup
- Okra: 184 mcg (46% DV) per cooked cup
- Fava beans: 177 mcg (44% DV) per cooked cup
- Turnip greens: 170 mcg (42% DV) per cooked cup
- Broccoli: 168 mcg (42% DV) per cooked cup
- Brussels sprouts: 157 mcg (39% DV) per cooked cup
- Beets: 136 mcg (34% DV) per cooked cup
- Hazelnuts: 130 mcg (32% DV) per cup
- Collard greens: 129 mcg (32% DV) per cooked cup
- Split peas: 127 mcg (31% DV) per cooked cup
- Chayote: 123 mcg (30% DV) per raw cup
- Escarole: 117 mcg (29% DV) per cooked cup
- Walnuts: 115 mcg (28% DV) per cup
- White potato: 114 mcg (28% DV) per large baked with skin
- Mustard greens: 105 mcg (26% DV) per cooked cup
- Broccoli: 103 mcg (25% DV) per cooked cup
- Corn: 103 mcg (25% DV) per canned cup
- Green peas: 101 mcg (25% DV) per cooked cup
- Cashews: 95 mcg (23% DV) per cup
- Parsley: 91 mcg (22% DV) per cup
- Parsnips: 90 mcg (22% DV) per cooked cup
- Durian: 87 mcg (21% DV) per cup
- Chinese broccoli: 87 mcg (21% DV) per cooked cup
- Guava: 81 mcg (20% DV) per cup
- Red potatoes: 81 mcg (20% DV) per large baked with skin
However, the folate levels of various foods can be affected by preparation methods.
For example, boiling folate-rich green vegetables can leech up to 49% of the folate into the cooking water, while steaming retains most of the nutrients (34).
In contrast, sprouting dried legumes can actually triple the folate availability, making them an excellent folate-rich food (35).
Frozen vegetables are a convenient and cost-effective option, but freezing initially reduces folate by about 25% and can lead to losses as high as 97% after 3 months in the freezer (36).
The best way to maximize your folate intake is to consume a variety of high-folate foods and to choose fresh, steamed vegetables whenever possible.
Folate Requirements
Only about 50% of natural folate found in food is bioavailable (able to be absorbed) (37, 38).
Folic acid, on the other hand, has higher bioavailability.
About 85% of folic acid is absorbed when consumed with a meal, while 100% is absorbed on an empty stomach (39, 40, 41).
Because folic acid is more easily absorbed, less is needed to meet daily requirements.
The RDA (Recommended Dietary Allowance) for folate takes these differences into account by expressing requirements as “dietary folate equivalents” (DFE) (39):
- 1 mcg of food folate = 1 mcg DFE
- 1 mcg of folic acid taken with food = 1.7 mcg DFE
- 1 mcg of folic acid taken on an empty stomach = 2 mcg DFE
Adults need 400 mcg DFE each day, which might look something like this:
- 400 mcg of folate from natural food sources
- OR 235 mcg of folic acid (from a supplement or fortified food) taken with food
- OR 200 mcg of folic acid (from a supplement or fortified food) taken on an empty stomach
- OR some combination of the above
During pregnancy and breastfeeding, folate needs are increased to 600 and 500 mcg DFE per day, respectively (40, 41). To meet these higher needs, supplements are often used.
Folic Acid: The Synthetic Form
The synthetic (man-made) form of folate is called folic acid, and it is found mainly in fortified or enriched foods and supplements.
The History of Folic Acid
Folic acid was first synthesized in the 1940s and was initially used to treat megaloblastic anemia caused by folate deficiency (42).
Compared to natural folate, folic acid was less expensive and more chemically stable, making it ideal for supplements (2).
However, it wasn’t until the 1960s that the use of folic acid supplements became widespread.
Around this time, scientists discovered that supplementing with folic acid could reduce the risk of neural tube defects (NTDs) in pregnancy (42, 43).
NTDs are severe birth defects, such as spina bifida and anencephaly, that occur when the neural tube fails to close during the early stages of fetal development (44).
In 1991, a large randomized controlled trial (RCT) found that women who took 4000 mcg of folic acid daily reduced their risk of having a pregnancy affected by an NTD by 70% (45).
Other studies showed that lower amounts of folic acid could also reduce the risk of NTDs, so it was eventually recommended that all women consume 400 mcg of dietary folate equivalents per day from food or supplements (39, 46, 47).
Unfortunately, most women weren’t consuming the recommended amount, so the FDA mandated that enriched grain products be fortified with folic acid in 1998 (48, 49).
After implementing these new rules, folate deficiency decreased to <2%, and the prevalence of NTDs in the United States was reduced by 20-50% (50, 51, 52).
Foods High in Folic Acid
Folic acid does NOT occur naturally in foods, but it is added to some processed foods.
In the United States, the FDA requires food manufacturers to add 140 mcg of folic acid to every 100 grams of “enriched” grain products (48, 53, 54).
“Enriched” products are foods that have had the nutrients lost during processing added back in, so that the final product is roughly nutritionally equivalent to the original (55).
In the US, most white bread, baked goods, cornmeal, white rice, white pasta, and refined breakfast cereals are enriched with folic acid.
It has been estimated that these fortified foods contribute an extra 100-200 mcg of folic acid per day to the average American’s diet (56, 57).
Non-Food Sources of Folic Acid
In addition to food, many people also take multivitamin-mineral supplements that contain folic acid.
While folic acid is not the best option for supplements (we’ll talk about this later), it is cheap and shelf-stable, so it is used by many inexpensive over the counter brands.
Doses in adult daily multivitamins are typically around 400 mcg (680 mcg DFE), which is above the RDA for folate (400 mcg DFE).
It is easy to see how people who take vitamins and eat folic acid enriched foods can easily surpass the recommended daily intake.
Structure & Metabolism of Folic Acid
Folate and folic acid have a few major differences:
- Oxidized vs Reduced: Natural folate is in the reduced form, whereas folic acid is in the oxidized form. (This is a fancy way of saying that folic acid has fewer hydrogen atoms than folate.)
- Poly vs mono glutamate: Natural folate is in the polyglutamate form and must be converted to the monoglutamate form before it can be absorbed, whereas folic acid is already a monoglutamate and can be absorbed as-is.
- Steps to activation: Activation of natural THF folate requires only 2 steps, whereas the activation of folic acid requires 4 steps (see below).
Studies show that at doses above 200 mcg per day, the DHFR enzyme can max out, leaving excess folic acid to be absorbed directly into the bloodstream (2).
Some of this unmetabolized folic acid heads to the liver where it can be converted to L-5-MTHF (58, 59).
However, the activity of the DHFR enzyme in the liver is relatively low, so unmetabolized folic acid can circulate in the bloodstream for a while before it is fully metabolized (60).
The Problem with Folic Acid
In countries that have implemented fortification, unmetabolized folic acid can be detected in up to of 95% of people tested (61, 62, 63).
Folic acid is only beneficial if it can be converted to the active form, L-5-MTHF, so high levels of unmetabolized folic acid may pose a problem.
Potential Health Risks of Too Much Folic Acid
Although more research is needed, some studies suggest that consuming too much folic acid may negatively impact our health.
1. It May Increase Cancer Risk
Around the time that the United States started fortifying foods with folic acid, there was an increase in the incidence of colon cancer (64).
Since then, many studies have shown increases in both prostate cancer and colon cancer in participants who take folic acid supplements (65, 66, 67).
However, this is only a correlation and does not prove causation. Other studies have shown no increase in cancer risk with folic acid supplementation (68, 69, 70).
Some researchers hypothesize that excessive folate may spur the growth of pre-existing cancers or precancerous growths since cancer cells grow rapidly and have a higher need for folate, but more research is needed (71, 72).
2. It May Reduce Immune Function
A few studies have looked at the relationship between immunity and folic acid (73, 74).
These studies found that circulating unmetabolized folic acid is linked to reduced natural killer cell activity – an important part of the innate immune system (75).
Much more research is needed to understand the significance of these findings, but it is certainly interesting.
Folate and Genetic Mutations
Earlier, we briefly mentioned the importance of the MTHFR enzyme in folate metabolism.
MTHFR is responsible for the last step in the activation of folate (converting 5,10-MTHF to L-5-MTHF) (76).
Mutations in the genes that code for MTHFR are fairly common and can impair this conversion (77, 78).
The most common MTHFR mutations are C677T and A1298C (79).
With the C677T mutation, the activity of MTHFR can be impaired by 35% in those who are heterozygous (one copy of the mutation) and up to 70% in those who are homozygous (two copies of the mutation) (80).
When MTHFR activity is impaired, folic acid can’t be activated as quickly, leading to higher levels of unmetabolized folic acid and lower levels of active folate in the blood (81, 82).
MTHFR mutations have been linked to increased risk of the following conditions:
- Alzheimer’s disease (83, 84)
- Cardiovascular disease (85, 86)
- Diabetic nephropathy (87, 88)
- Infertility (89, 90)
- Migraines (91, 92, 93)
- Neural tube defects (94)
- Parkinson’s disease (95, 96)
- Psoriasis (97, 98)
People who have the MTHFR mutation may benefit from avoiding foods that contain folic acid and choosing supplements L-5-MTHF, the already active form of folate (99, 100).
How to Choose the Right Folate Supplement
Supplements that use the active form of folate (L-5-MTHF) are generally preferred over those containing folic acid.
Studies have shown that L-5-MTHF is well absorbed and can raise folate levels as well as or even more effectively than folic acid (101, 102, 103).
To make sure you’re getting a supplement that contains L-5-MTHF, check the label for any of the following (104):
- Metafolin
- Quatrefolic
- Levomefolic acid
- L-methylfolate
- L-5-MTHF
- 5-MTHF
These are alternative names for L-5-MTHF, so any supplement that uses one of the above is usually a good choice.
Benefits of L-5-MTHF Over Folic Acid
Supplements that contain methylated folate (L-5-MTHF) are better than folic acid for the following reasons (2):
1. Less likely to mask a vitamin B12 deficiency.
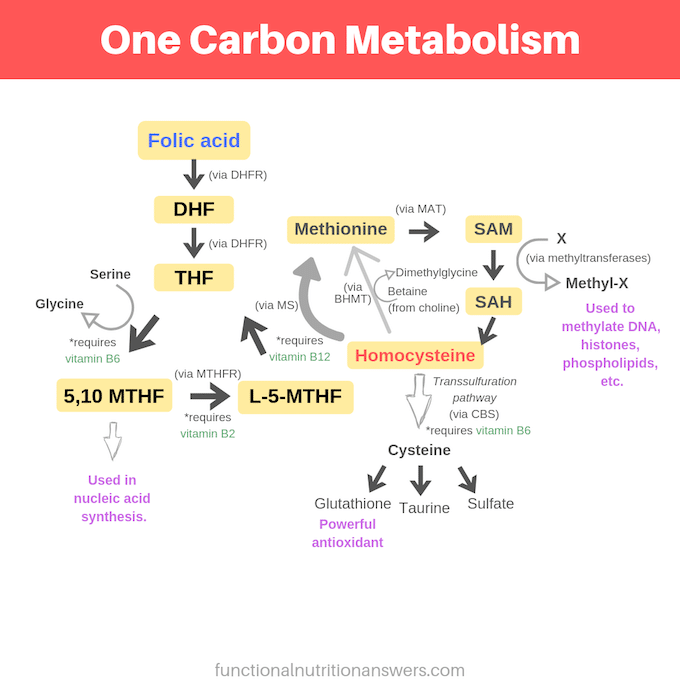
High doses of folic acid supplementation can “mask” a vitamin B12 deficiency by preventing the development of megaloblastic anemia (see graphic below for more details).
This is not good since B12 deficiency can still cause neurological damage, even if someone doesn’t know they have it.
For many people, the presence of megaloblastic anemia is the 1st sign of B12 deficiency.
If someone is B12 deficient, but megaloblastic anemia never develops because of folic acid supplements, the deficiency may go unnoticed until more severe signs, like nerve damage, occur.
This is of particular concern in older adults since vitamin B12 malabsorption is much more common in that age group (105).
Because of this concern, the Institute of Medicine has advised adults to not take more than 1000 mcg (1 mg) of folic acid per day, and some researchers argue this should be lowered to 500 mcg per day (106).
However, the active form of folate (L-5-MTHF) does NOT mask megaloblastic anemia caused by vitamin B12 deficiency.
This is because without vitamin B12, L-5-MTHF cannot be converted back into the form used in DNA synthesis, so megaloblastic anemia will still develop.
Thus, if L-5-MTHF is being taken as a supplement and megaloblastic anemia is present, it is most likely due to a vitamin B12 deficiency.
2. Still works for those taking DHFR inhibiting medications.
A second reason why folate supplements are superior to folic acid is that they still work for people who are taking medications that interfere with the DHFR enzyme.
DHFR is the enzyme that converts folic acid into the intermediate forms DHF and THF.
Methylated folate doesn’t require these enzymes since it is already in the active form. Therefore, even people on DHFR-blocking medications can properly utilize it.
Examples of medications that can interfere with the DHFR enzyme include (2):
- Antiparasitics like pyrimethamine.
- Diuretics like triamterene.
- Folate-inhibiting antibiotics like trimethoprim.
- Immunosuppressants and chemotherapeutics like methotrexate and aminopterin.
3. Suitable for people with MTHFR mutations.
As discussed previously, some people have genetic mutations that impair MTHFR activity and the ability to convert folate to its active form.
For these people, supplementing with folic acid (or even an intermediate form like folinic acid) may not be very helpful, since their bodies will struggle to convert it to L-5-MTHF.
This poor conversion may also result in higher amounts of circulating unmetabolized folic acid, which has been associated with negative health outcomes.
However, taking L-5-MTHF directly bypasses the MTHFR enzyme and provides the body with active folate that it can use right away.
For this reason, people with MTHFR mutations often choose supplements that contain L-5-MTHF rather than folic acid.
Our Favorite Folate-Containing Supplements
There are hundreds of folate supplements to choose from, so we’ve compiled a list of our favorite high-quality products.
Please note that as an Amazon Associate I earn from qualifying purchases.
Folate-Containing Multivitamin:
Pure Encapsulations O.N.E. Multivitamin
For a high-quality multivitamin/mineral that contains L-5-MTHF, Pure Encapsulations is a great choice.
In this supplement, you’ll find 400 mcg of L-5-MTHF (667 mcg DFE) per capsule, along with other nutrients.
This product can be purchased online here.
Folate-Containing Gummies:
Smarty Pants Complete
Smarty Pants has several gummy multivitamins for men, women, and children, all of which contain methylated folate, rather than folic acid.
Six of the adult chewable gummies provide 400 mcg of L-methylfolate calcium salt.
Smarty Pants make a good option for those who cannot swallow pills and can be purchased online here.
It is important to note that these gummies do not contain important minerals like calcium, magnesium, or selenium, so an additional multimineral supplement may be needed.
Folate Lozenges or Drops:
Seeking Health
Another option for those who experience difficulty swallowing pills is drops or lozenges, which are available through Seeking Health.
These products can be purchased online here and here.
Folate-Containing Prenatal:
Seeking Health Optimal Prenatal
Seeking Health also makes a wonderful prenatal that contains L-methylfolate (in the form of Quatrefolic), along with other important nutrients like choline.
However, it is important to note that it does not contain some minerals, iron, or DHA, so additional supplementation may be needed.
Seeking Health Optimal Prenatal can be purchased online here.
Precautions with Supplementation
It is important to remember that nutrients do not exist in a vacuum, and many other vitamins and nutrients are needed for proper methylation and one-carbon metabolism.
While some people who discover they have an MTHFR mutation may jump straight into high dose supplementation with methylated folate, this is not always a good idea.
Overloading yourself with folate without knowing whether you are deficient in other important methylation nutrients or without having functional labs to guide you could be a recipe for trouble.
Working with a dietitian or other qualified healthcare practitioner is always recommended before beginning a new supplement or dramatically changing your diet.
Your practitioner will analyze your health history and current diet, lifestyle, and medications to provide custom recommendations just for you.
Final Thoughts
Vitamin B9 is an important nutrient for one-carbon metabolism, DNA synthesis, and amino acid metabolism.
Deficiency can lead to megaloblastic anemia and is associated with an increased risk of cancer and other diseases.
There are two main forms of vitamin B9: folate (the natural form) and folic acid (the synthetic form).
Both must be converted to the active form, L-5-MTHF, in order to be used by the body, but folic acid requires more conversions and therefore can be more difficult for the body to use.
If too much is consumed, excess folic acid can build up in the blood and may have negative effects on health.
Additionally, some people also have genetic mutations that impair the MTHFR enzyme, making it even more difficult to activate folic acid.
For these reasons, it’s generally best to consume folate from food or through supplements containing L-5-MTHF, rather than folic acid.
Want to save this article? Click here to get a PDF copy delivered to your inbox.

Amy is a registered dietitian nutritionist and experienced nutrition editor. She received her Masters in Nutrition Diagnostics from Cox College and her Bachelors in Dietetics from Missouri State University. She currently works as a nutrition editor for Healthline and Greatist. Her passion is finding ways to communicate nutrition research in an interesting and easy-to-understand way.
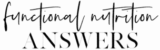



thank you
want to ask about patients with high risk to get NTD or already have history with NTD
for these patient what is your recommendation ?
until know the all recommendation go to take 5 mg of folic acid .
do you have recommendation to take folate ? how much the daily dose ?
This is wonderful information but I notice the references have not been included (and there are many). Does the download version include these as I am interested in reviewing the ones regarding cooking impact.
Thank you so much!
No, but you can click any of the reference numbers to open up the articles on pubmed and then use whatever tool you’d like to access the full text!
You did a wonderful job on this! Very thorough.
Wow! A ton of work went into this, I can tell. Great job!
Fantastic information and presented so well! great job on the hard work
Such a fantastic overview! I love the way your organized this 🙂
Wow, as always so thorough and well organized! Definitely bookmarking this to revisit again and again!